Primary Endpoint - “Off” Time
Primary Endpoint
NOURIANZ® is the first and only adjunct therapy that reduces “off” time
by lifting the brake of adenosine1,2
Study description: Randomized, 12-week, multicenter, double-blind, placebo-controlled studies of NOURIANZ 20 mg and 40 mg as adjunctive treatment to levodopa treatment in patients with PD (mean age=65 years) experiencing “off” time (mean approximately 6 hours/day).
In Studies 1 & 2, patients were randomized to once-daily treatment with NOURIANZ 20 mg, 40 mg, or placebo with the primary endpoint of change from baseline in % of awake time spent in the “off” state:
- Study 1 (N=195) was conducted in the U.S. and Canada
- Study 2 (N=225) was conducted in the U.S.
In Studies 3 & 4, patients were randomized equally to treatment with NOURIANZ 20 mg, 40 mg, or placebo with the primary endpoint of change from baseline spent in “off” time/day
- Study 3 (N=357) was conducted in Japan
- Study 4 (N=366) was conducted in Japan
Secondary endpoint in all 4 studies was change from baseline in “on” time without troublesome dyskinesia. Endpoints measured using 24-hour patient diaries.1,2
All enrolled patients were on stable doses of baseline therapy for the duration of the studies. Baseline therapy was levodopa/carbidopa (Studies 1, 2, 3, and 4) or levodopa/benserazide (Studies 3 and 4) for all patients with or without other concomitant baseline medications for PD, including dopamine agonists (85%), COMT inhibitors (38%), MAO-B inhibitors (40%), anticholinergics (13%), and/or amantadine (33%).1,2
COMT, catechol-o-methyl transferase; MAO, monoamine oxidase.
Based on 24-hour patient diaries in Studies 3 & 4: NOURIANZ reduced “off” time1,3
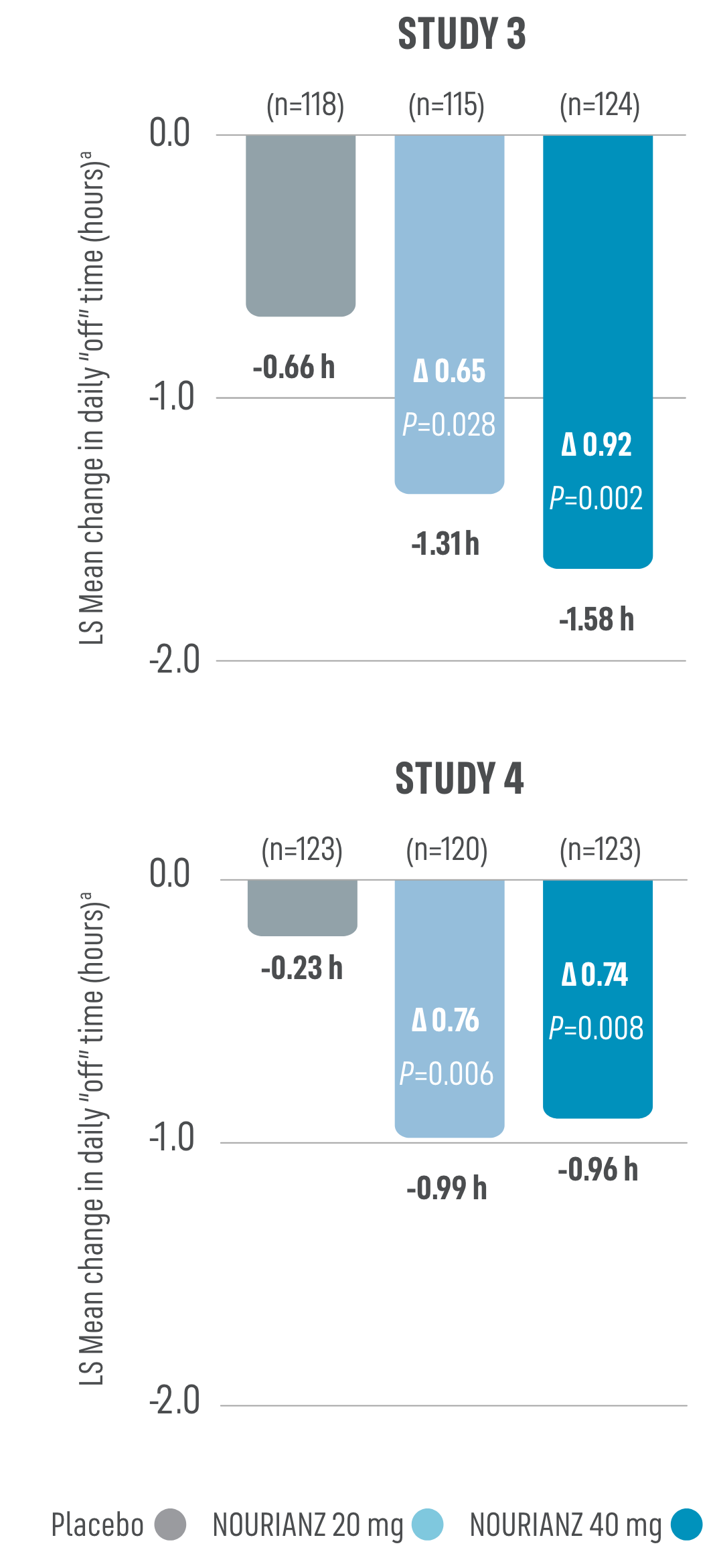
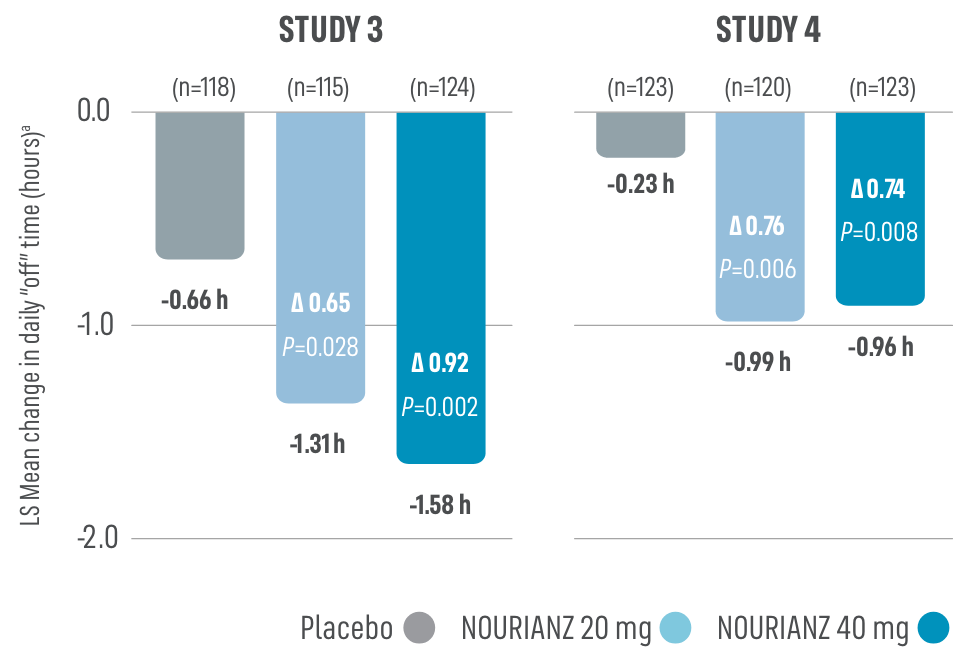
aLeast squares (LS) mean change from baseline (ANCOVA).
ANCOVA, analysis of covariance.
- At Week 12, patients taking NOURIANZ in clinical trials saw a significant decrease in “off” time from baseline compared to placebo in all 4 studies (N=1,143 PD patients)1
Studies 1 and 2: Change in “off” time from baseline to endpoint (12 weeks),
daily awake “off” time (% of awake hours)1,3
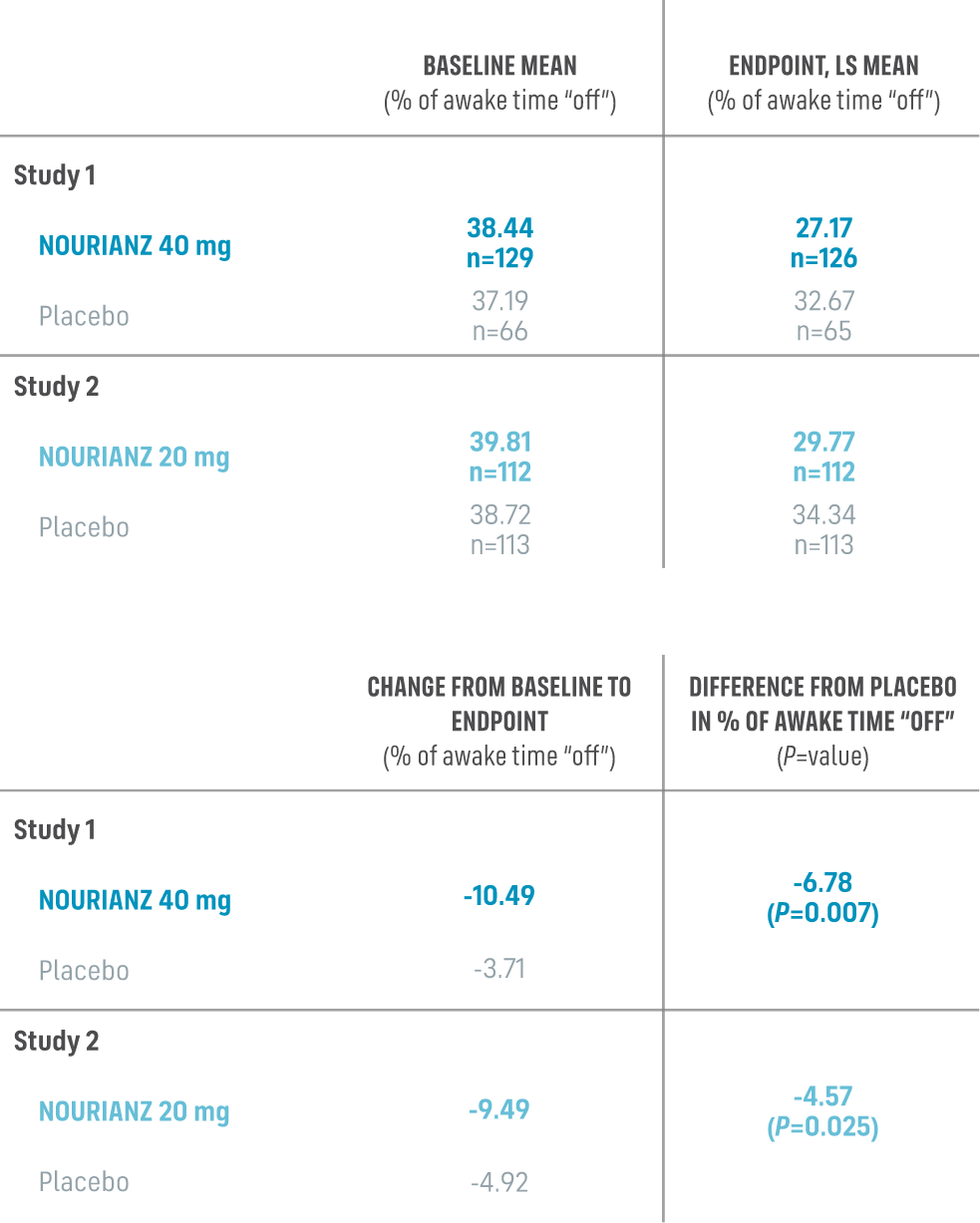
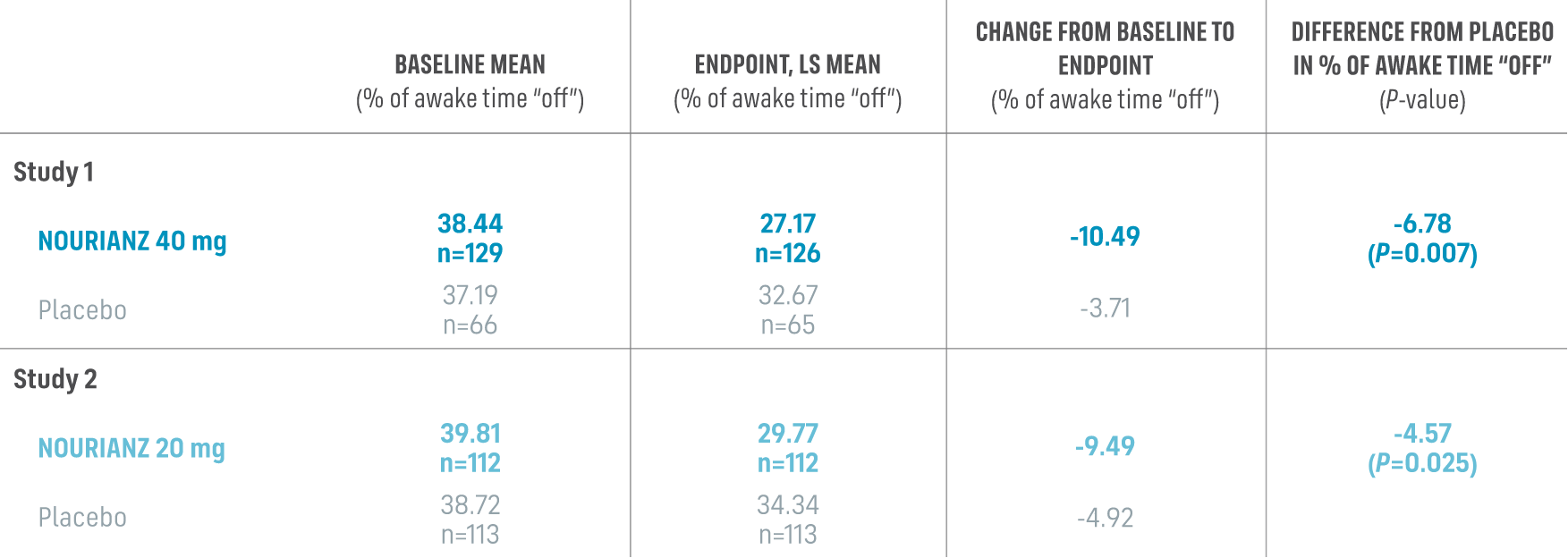
- Pre-specified analysis for Study 1 was ANOVA, and for Study 2 was ANCOVA*
*Least squares mean change from baseline (ANOVA in Study 1, ANCOVA in Study 2).
ANOVA, analysis of variance; ANCOVA, analysis of covariance.
Secondary Endpoint - “On” Time
Secondary Endpoint
NOURIANZ lifts the brake of adenosine to help increase good “on” time1,2*
Based on 24-hour patient diaries: NOURIANZ reduced “off” time and was shown to increase good “on” time without troublesome dyskinesia at Week 121,3*
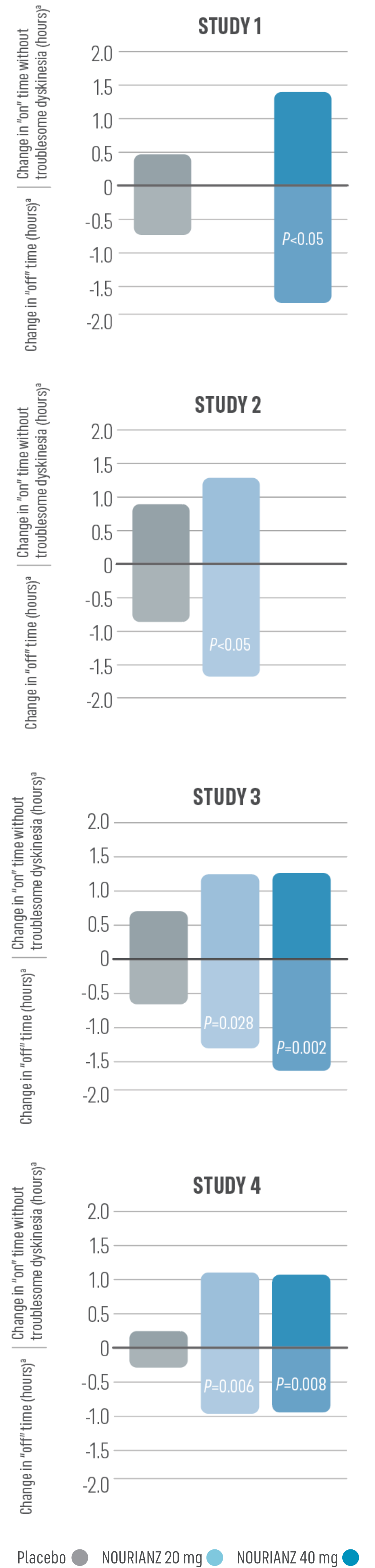
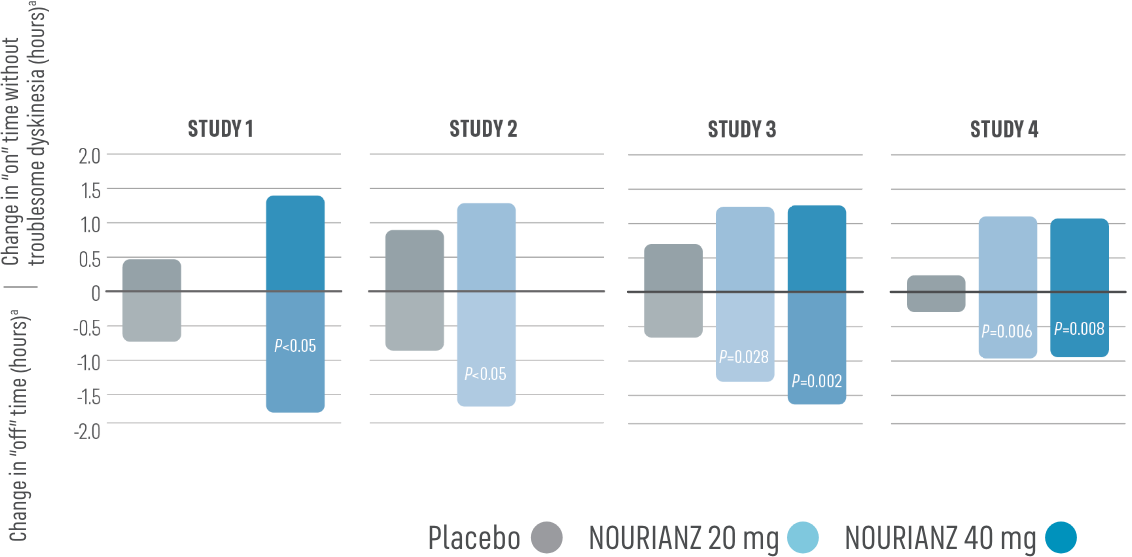
*Good “on” time=“on” time without troublesome dyskinesia plus “on” time with non-troublesome dyskinesia.
aLeast squares mean change from baseline (ANOVA in Study 1, ANCOVA in Studies 2, 3, and 4).
ANOVA, analysis of variance; ANCOVA, analysis of covariance.
Baseline therapy was levodopa/carbidopa and/or levodopa/benserazide for all patients with or without
other concomitant medications for PD.
- At Week 12, patients treated with NOURIANZ experienced an increase in good “on” time.1,3*
-
- A change from baseline in good “on” time without troublesome dyskinesia (i.e., “on” time without dyskinesia plus “on” time with non-troublesome dyskinesia) was a secondary efficacy endpoint
- Increases from baseline with NOURIANZ 20 mg ranged from 0.90 to 1.35 hours. Nominal P-values: P=0.135 in Study 2; P=0.085 in Study 3; P=0.008 in Study 4
- Increases from baseline with NOURIANZ 40 mg ranged from 0.85 to 1.45 hours. Nominal P-values: P=0.026 in Study 1; P=0.048 in Study 3; P=0.008 in Study 4
- Increases from baseline with placebo ranged from 0.28 to 0.80 hours
NOURIANZ in combination with levodopa may cause dyskinesia or exacerbate pre-existing dyskinesia.
NOURIANZ was evaluated in patients taking levodopa treatment with or without
other concomitant baseline medications for PD1,3
Other concomitant medications for PD taken in NOURIANZ clinical trials.
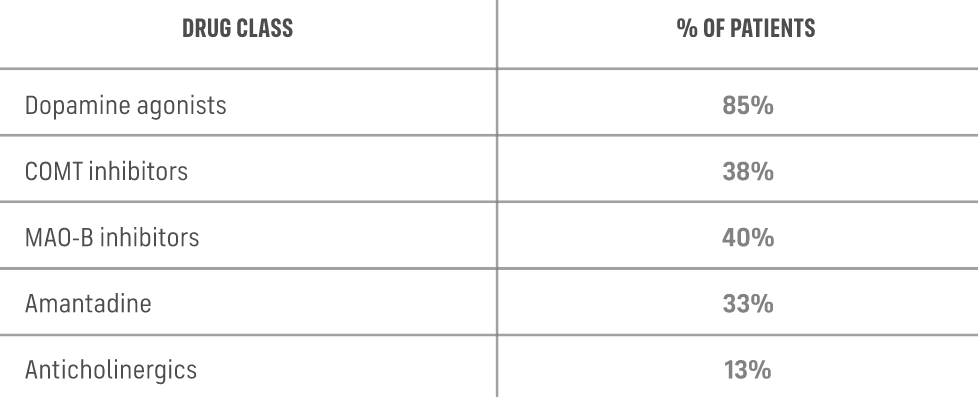
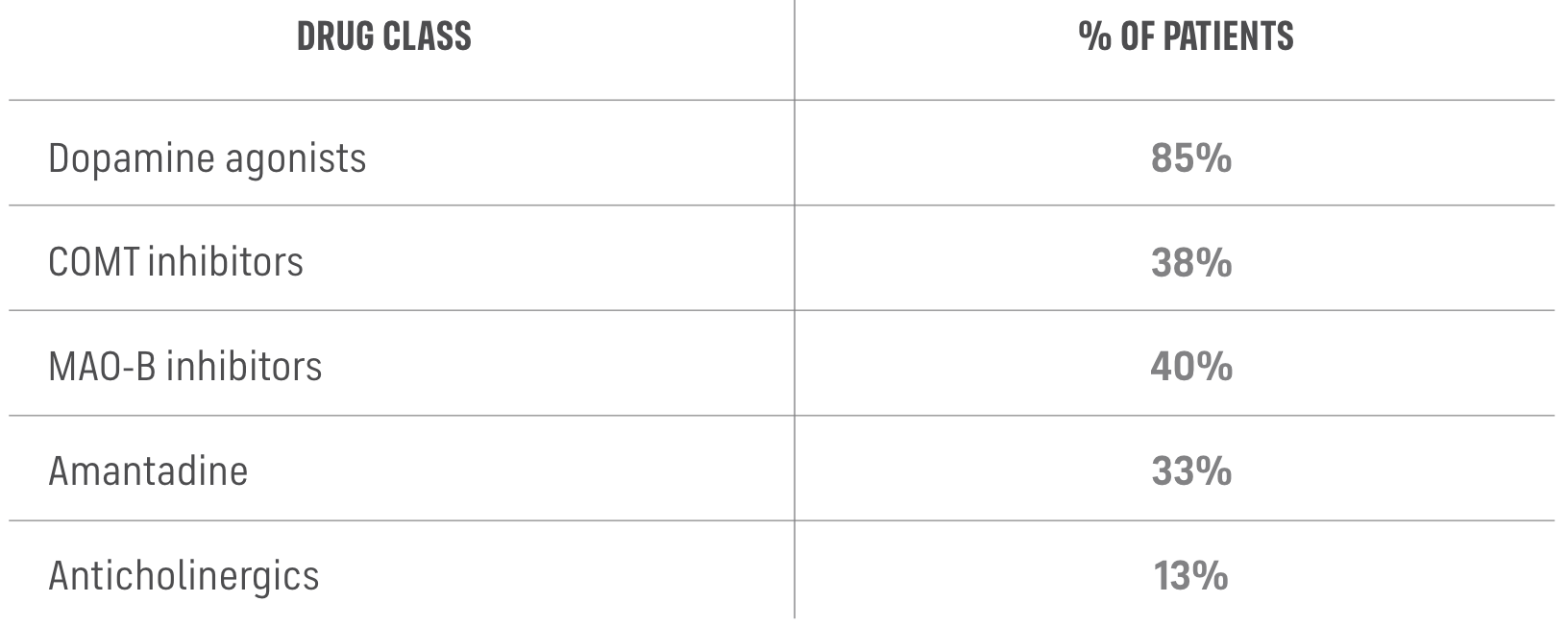


COMT, catechol-o-methyltransferase; MAO-B, monoamine oxidase B.
Actor Portrayals.
Actor Portrayals.
Indication
NOURIANZ® (istradefylline) is an adenosine receptor antagonist indicated as adjunctive treatment to levodopa/carbidopa in adult patients with Parkinson’s disease (PD) experiencing “off” episodes.
Important Safety Information
Warnings and Precautions
Dyskinesia: NOURIANZ in combination with levodopa may cause dyskinesia or exacerbate pre-existing dyskinesia. In clinical trials, 1% of patients treated with either NOURIANZ 20 mg or 40 mg discontinued treatment because of dyskinesia, compared to 0% for placebo.
Hallucinations / Psychotic Behavior: Because of the potential risk of exacerbating psychosis, patients with a major psychotic disorder should not be treated with NOURIANZ. Consider dosage reduction or discontinuation if a patient develops hallucinations or psychotic behaviors while taking NOURIANZ.
Impulse Control / Compulsive Behaviors: Patients treated with NOURIANZ and one or more medication(s) for the treatment of Parkinson’s disease (including levodopa) may experience intense urges to gamble, increased sexual urges, intense urges to spend money, binge or compulsive eating, and/or other intense urges, and the inability to control these urges. In clinical trials, 1 patient treated with NOURIANZ 40 mg was reported to have impulse control disorder, compared to no patient on NOURIANZ 20 mg or placebo.
Drug Interactions
The maximum recommended dosage in patients taking strong CYP3A4 inhibitors is 20 mg once daily. Avoid use of NOURIANZ with strong CYP3A4 inducers.
Specific Populations
Pregnancy: Based on animal data, may cause fetal harm.
Hepatic impairment: The maximum recommended dosage of NOURIANZ in patients with moderate hepatic impairment is 20 mg once daily. Avoid use in patients with severe hepatic impairment.
Adverse Reactions
The most common adverse reactions with an incidence ≥5% and occurring more frequently than with placebo were dyskinesia (15%, 17%, and 8%), dizziness (3%, 6%, and 4%), constipation (5%, 6%, and 3%), nausea (4%, 6%, and 5%), hallucination (2%, 6%, and 3%), and insomnia (1%, 6%, and 4%) for NOURIANZ 20 mg, 40 mg, and placebo, respectively.
You are encouraged to report suspected adverse reactions to Kyowa Kirin, Inc. at 1-844-768-3544 or FDA at
1-800-FDA-1088 or www.fda.gov/medwatch.
Please see full Prescribing Information for NOURIANZ.
References: 1. NOURIANZ. Prescribing Information. Kyowa Kirin, Inc; 2023. Accessed November 1, 2023. https://www.nourianzhcp.com/assets/pdf/nourianz-full-prescribing-information.pdf. 2. Kalia LV, Brotchie JM, Fox SH. Novel nondopaminergic targets for motor features of Parkinson’s disease: review of recent trials. Mov Disord. 2013;28(2):131-144.
References: 1. Kalia LV, Brotchie JM, Fox SH. Novel nondopaminergic targets for motor features of Parkinson's disease: review of recent trials. Mov Disord. 2013;28(2):131-144. 2. Mori A. Mode of action of adenosine A2A receptor antagonists as symptomatic treatment for Parkinson’s disease. Int Rev Neurobiol. 2014;119:87-116. 3. Varani K, Vincenzi F, Tosi A, et al. A2A adenosine receptor overexpression and functionality, as well as TNF-α levels, correlate with motor symptoms in Parkinson’s disease. FASEB J. 2010;24(2):587-598. doi:10.1096/fj.09-141044. 4. Fuxe K, Marcellino D, Genedani S, Agnati L. Adenosine A2A receptors, dopamine D2 receptors and their interactions in Parkinson's disease. Mov Disord. 2007;22(14):1990-2017. doi: 10.1002/mds.21440. 5. Morelli M, Di Paolo T, Wardas J, Calon F, Xiao D, Schwarzschild MA. Role of adenosine A2A receptors in parkinsonian motor impairment and L-DOPA-induced motor complications. Prog Neurobiol. 2007;83(5):293-309. 6. Morelli M, Blandini F, Simola N, Hauser RA. A2A receptor antagonism and dyskinesia in Parkinson's disease. Parkinsons Dis. 2012;2012:489853. doi: 10.1155/2012/489853. 7. Mishina M, Ishiwata K. Adenosine receptor PET imaging in human brain. Int Rev Neurobiol. 2014;119:51-69. doi:10.1016/B978-0-12-801022-8.00002-7. 8. The voice of the patient: Parkinson’s disease. Silver Spring, MD: US Food and Drug Administration; April 2016. https://www.fda.gov/media/124392/download. Accessed June 11, 2019. 9. Hickey P, Stacy M. Available and emerging treatments for Parkinson’s disease: a review. Drug Des Devel Ther. 2011;5:241-254. 10. Stocchi F, Antonini A, Barone P, et al. Early DEtection of wEaring off in Parkinson disease: the DEEP study. Parkinsonism Relat Disord. 2014;20(2):204-211.
References: 1. NOURIANZ. Prescribing Information. Kyowa Kirin, Inc; 2020. Accessed April 1, 2021. https://www.nourianzhcp.com/assets/pdf/nourianz-full-prescribing-information.pdf 2. Kalia LV, Brotchie JM, Fox SH. Novel nondopaminergic targets for motor features of Parkinson’s disease: review of recent trials. Mov Disord. 2013;28(2):131-144. 3. Jenner P. Istradefylline, a novel adenosine A2A receptor antagonist, for the treatment of Parkinson’s disease. Expert Opin Investig Drugs. 2005;14(6):729-738. 4. Brichta L, Greengard P, Flajolet M. Advances in the pharmacological treatment of Parkinson’s disease: targeting neurotransmitter systems. Trends Neurosci. 2013;36(9):543-554. 5. Kaakkola S, Wurtman RJ. Effects of COMT inhibitors on striatal dopamine metabolism: a microdialysis study. Brain Res. 1992;587(2):241-249. 6. Kong P, Zhang B, Lei P, et al. Neuroprotection of MAO-B inhibitor and dopamine agonist in Parkinson disease. Int J Clin Exp Med. 2015;8(1):431-439. 7. Ossola B, Schendzielorz N, Chen SH, et al. Amantadine protects dopamine neurons by a dual action: reducing activation of microglia and inducing expression of GDNF in astroglia. Neuropharmacology. 2011;61(4):574-582. 8. Rubí B, Maechler P. Minireview: new roles for peripheral dopamine on metabolic control and tumor growth: let’s seek the balance. Endocrinology. 2010;151(12):5570-5581. doi:10.1210/en.2010-0745. 9. Gerlach M, Double K, Arzberger T, Leblhuber F, Tatschner T, Riederer P. Dopamine receptor agonists in current clinical use: comparative dopamine receptor binding profiles defined in the human striatum. J Neural Transm (Vienna). 2003;110(10):1119-1127. 10. Ishibashi K, Miura Y, Wagatsuma K, Toyohara J, Ishiwata K, Ishii K. Adenosine A2A receptor occupancy by long-term istradefylline administration in Parkinson’s disease. Mov Disord. 2021;36(1):268-269. doi:10.1002/mds.28378.
References: 1. NOURIANZ. Prescribing Information. Kyowa Kirin, Inc; 2020. Accessed April 1, 2021. https://www.nourianzhcp.com/assets/pdf/nourianz-full-prescribing-information.pdf 2. Kalia LV, Brotchie JM, Fox SH. Novel nondopaminergic targets for motor features of Parkinson’s disease: review of recent trials. Mov Disord. 2013;28(2):131-144. 3. Data on file. Kyowa Kirin Pharmaceutical Development, Inc., Princeton, NJ.
References: 1. NOURIANZ. Prescribing Information. Kyowa Kirin, Inc; 2020. Accessed April 1, 2021. https://www.nourianzhcp.com/assets/pdf/nourianz-full-prescribing-information.pdf 2. Data on file. Kyowa Kirin Pharmaceutical Development, Inc., Princeton, NJ.
Reference: 1. NOURIANZ. Prescribing Information. Kyowa Kirin, Inc; 2020. Accessed April 1, 2021. https://www.nourianzhcp.com/assets/pdf/nourianz-full-prescribing-information.pdf
Reference: 1. NOURIANZ. Prescribing Information. Kyowa Kirin, Inc; 2020. Accessed April 1, 2021. https://www.nourianzhcp.com/assets/pdf/nourianz-full-prescribing-information.pdf